What is Pelvic Organ Prolapse?
Pelvic organ prolapse (POP) occurs when a pelvic organ, such as yourbladder, uterus, rectum, or small intestine drops (prolapses) from its original position, and herniates into the vagina or rectum. It is generally secondary to changes in integrity of the ligaments and supporting connective tissue structures. Generally the pelvic floor muscles are found to be affected in these situations with poor recruitment, weakness and/or altered tone. Prolapse affects 50% of women that have had children. Approximately 11% of all females require at least one corrective surgical procedure during their lifetime. Types of prolapse include:
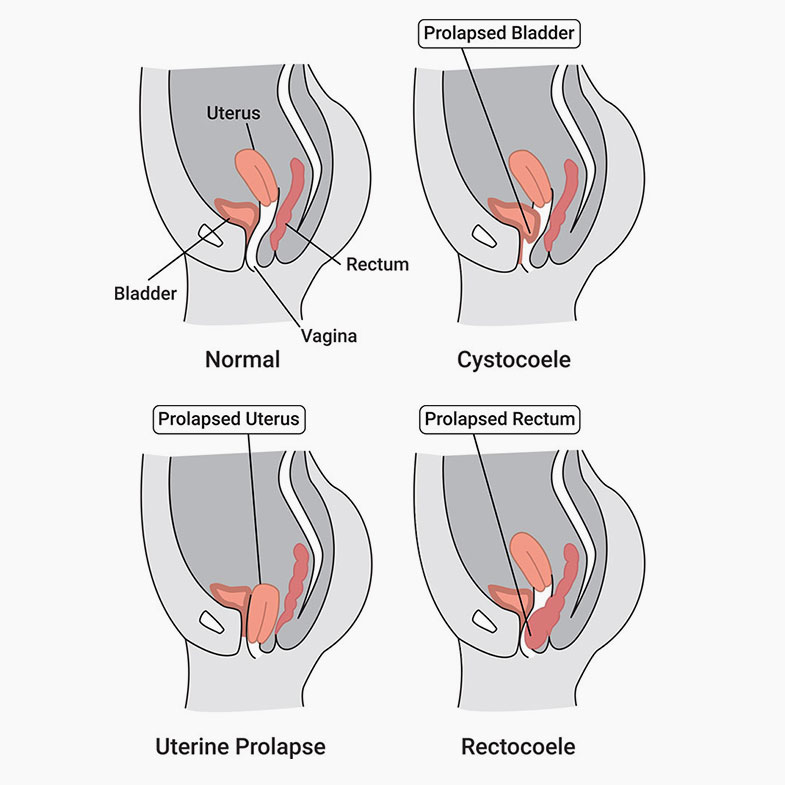
Cystocele: A cystocele is the descent of the bladder into the vagina. This generally is due.
to a weakening or defect in the front/anterior wall of the vagina. Some of the most common causes of this condition are chronic straining with bowel movements, chronic coughing, child birth and obesity.
Urethrocele: A urethrocele is the descent of the urethra into the vagina. It is often seen with cystoceles. Urethroceles are often caused during childbirth occurring as the baby moves through the vagina causing damage to the surrounding tissues. When they occur in women who have never had children, they may be the result of a congenital weakness in the tissues of the pelvic floor.
Rectocele: A rectocele is the protrusion of the rectum into the back wall of the vagina. Often this means there is a weakening or defect in the back/posterior vaginal wall, allowing the rectum to protrude into the vagina. Some of the most common causes of this condition are chronic holding of stool, straining with bowel movements, childbirth, and obesity.
Uterine Prolapse: A uterine prolapse refers to the descent of the uterus into the vagina. Women report the sensation of heaviness in the pelvic floor or perineum, the sense of something sagging or the presence of something lodged in the vagina or the sensation of a lump in the vagina. Some of the most common causes of this condition are chronic holding and straining for stool, difficult or multiple vaginal deliveries, obesity, and chronic coughing.
Vaginal Vault Prolapse: Occurs when the top of the vagina descends down into the vaginal vault. It occurs most often in women who have had a hysterectomy. Women report a bulging sensation in the vagina.
Enterocele: An enterocele is the descent of the small intestine into the vagina. It has the potential to interfere with ease of bowel movements by causing obstruction because of it’s positioning. It more commonly occurs in women who have had a hysterectomy.
Rectal Prolapse: A rectal prolapse occurs when part of the large intestine’s lowest section (the rectum) slips outside the anus. The prolapsed rectum can cause difficulty with evacuating stool and possibly fecal incontinence.

